Clinical Trial Spotlight: A Phase 1, Dose Escalation Study of Intravenous TK216 in Patients with Relapsed or Refractory Ewing Sarcoma
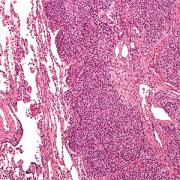
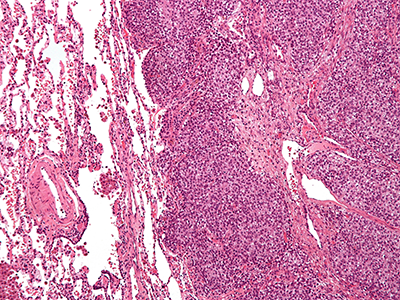
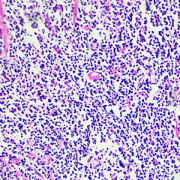
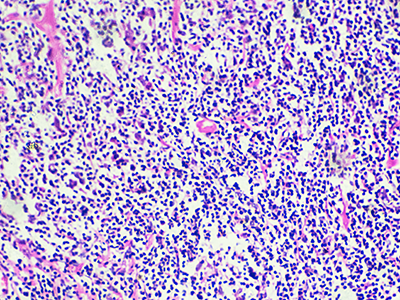
Despite advances in chemotherapy, the outcome for metastatic or relapsed Ewing sarcoma (ES) is dismal. ES harbors a pathognomonic translocation EWS-FLI1, leading to an oncogenic fusion protein that drives its development and for years has been considered an undruggable target. TK216 is a unique, investigational agent that targets EWS-FLI1 by disrupting its binding to RHA, a protein partner needed for the activity of EWS-FLI1, and one of the first in class to do so. In pre-clinical models of ES, there was cell death and inhibition of tumor growth which was potentiated with vincristine.
Study TK216-01 is a Phase 1 study of TK216 in patients with relapsed or refractory Ewing sarcoma currently open at a limited number of sites. The initial Phase 1 data demonstrates this drug has been generally well tolerated with encouraging preliminary data in patients. The study is currently in the expansion cohort using the recommended phase 2 dose of TK216 in combination with vincristine and is open to enrollment at Children’s National.
“There was interesting preliminary data presented at the CTOS meeting last November,” says AeRang Kim, M.D., Ph.D., a pediatric oncologist at Children’s National and the study’s principal investigator. “This really is a first-in-class that targets this specific translocation which makes it an exciting option for this patient group.”
Children’s National Hospital is the only pediatric center in the Washington, D.C., region to offer this trial.
TK216 in Patients with Relapsed or Refractory Ewing Sarcoma
- PI: AeRang Kim, M.D., Ph.D.
- Status: Recruiting
For more information about this trial, contact:
Ann Liew, M.S., CCRP
202-476-6755
aliew@childrensnational.org
Click here to view Open Phase 1 and 2 Cancer Clinical Trials at Children’s National.
The Children’s National Center for Cancer and Blood Disorders is committed to providing the best care for pediatric patients. Our experts play an active role in innovative clinical trials to advance pediatric cancer care. We offer access to novel trials and therapies, some of which are only available here at Children’s National. With research interests covering nearly every aspect of pediatric cancer care, our work is making great advancements in childhood cancer.