Study finds new genetic cause of neurodevelopmental disorders
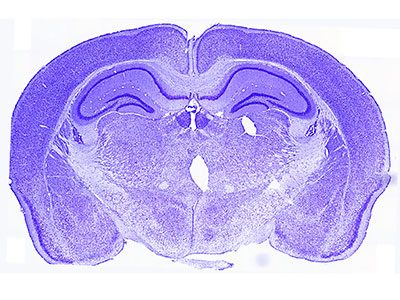
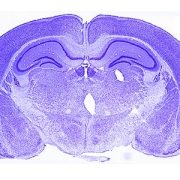
Nissel staining of pre-clinical model brain.
A cross-disciplinary team of researchers and physicians from Children’s National Hospital and Washington University School of Medicine in St. Louis, in collaboration with physicians from around the world, identified a new genetic cause of neurodevelopmental disorders (NDDs). In a new study published in the American Journal of Human Genetics, researchers found 14 unrelated patients with 15 different sequence variants in HECTD1 – 10 missense, 3 frameshift, 1 nonsense and 1 splicing variant – with NDDs, including autism, attention-deficit/hyperactivity disorder (ADHD) and epilepsy.
Moving the field forward
Many patients suspected of having a genetic disorder remain undiagnosed. In about 10% of these cases, the genetic change is in a gene unknown to cause the disorder.
“Describing a new genetic cause of neurodevelopmental disorders will allow for the characterization of the gene’s role in brain development, the genetic syndrome and the mechanisms of disease,” says Irene Zohn, PhD, principal investigator in the Center for Genetic Medicine Research at Children’s National and co-lead of the study. “This information will lead to developing treatments to improve the lives of patients.”
The patient benefit
“Our study represents the first report of HECTD1 in NDDs,” says Dr. Zohn. “Now that this gene is linked to the disorder, clinicians with patients with sequence variation in this gene can enroll in studies to understand this new HECTD1 syndrome.”
Proper genetic diagnosis is important so that comorbidities and the natural history of the disorder can be described, which will lead to improvements in patient care.
What we hope to discover
Now that a new genetic syndrome has been defined, researchers hope to establish how prevalent the syndrome is and describe its features. Using pre-clinical models, they’ll continue to study the developmental basis of the disorder and the molecular mechanisms to develop therapies.
Children’s National leads the way
The HECTD1 gene was discovered in Dr. Zohn’s laboratory, and her research team connected with Christina Gurnett, MD, PhD, co-lead of the study from Washington University School of Medicine, to link this gene to human disease.
Additional authors from Children’s National include – Elias Oxman, Keito Ishibashi, Sonia Sebaoui, Kathryn Luedtke, Bryce Winrow, Seth Berger, MD, PhD, Christina L. Grant, MD, PhD, and Joshua Corbin, PhD.
You can read the full study Sequence Variants in HECTD1 Result in a Variable Neurodevelopmental Disorder in the American Journal of Human Genetics.