Assessing the risk factors in rheumatic heart disease
Rheumatic heart disease is caused by untreated throat infections from the streptococcal bacterium. The infections progress into acute rheumatic fever and eventually weaken the valves of the heart.
Rheumatic heart disease (RHD) is the most commonly acquired cardiovascular disease in children and young adults. The devastating condition, which was endemic in the United States before 1950, is now relatively rare in the developed world due to social and economic development and the introduction of penicillin. But, in the developing world RHD remains nearly as common as HIV.
Fortunately, RHD is a cumulative disease and opportunities exist for early intervention. To further explore the utility of early diagnosis and intervention, a research team headed by Children’s National Heart Institute cardiologist Andrea Beaton, M.D., conducted a prospective natural history study of children with latent RHD.
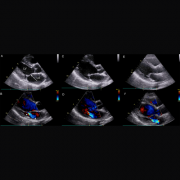
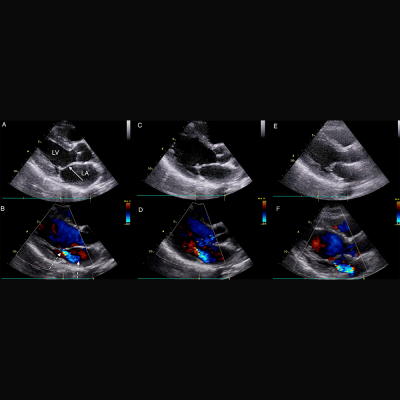
RHD is caused by untreated streptococcal throat infections that progress into acute rheumatic fever (ARF) and eventually weaken the valves of the heart. While initial episodes of ARF occur almost exclusively during childhood, RHD most commonly presents in adolescents and young adults. This latent period between ARF and clinically apparent RHD is an ideal opportunity for early intervention, and screening echocardiography (echo) has emerged as a potentially powerful tool for early detection of RHD.
In their study published in the journal Circulation in September 2017, Dr. Beaton and her colleagues examined echocardiograms from children with latent RHD who were enrolled in the Ugandan National RHD registry. The researchers also developed models to search for risk factors and compare progression-free survival between patients who did and did not receive penicillin.
The team reports that children with moderate-to-severe latent RHD discovered by echo screening have poor outcomes. Children with both borderline and mild definite RHD have better outcomes but remain at substantial risk of progression. The researchers also found that children who are diagnosed at a younger age, and the presence of morphological mitral valve features, generally lead to unfavorable outcomes.
The authors conclude that children with moderate to severe RHD at screening should be considered for treatment as clinically diagnosed RHD, and that children with borderline or mild definite RHD at screening should, at a minimum, be maintained in close clinical follow up.
“It is clear that children found to have the earliest forms of RHD, seen only by echo, are at substantial risk for progression of disease. This study urges us forward to see if we can intervene to stop this progression once children are identified,” says Dr. Beaton. “We are excited that our next project will be to do just that – a randomized clinical trial in Uganda to determine if penicillin can protect the hearts of children found to have latent RHD.”