H-IPSE internalized by just a limited range of cells
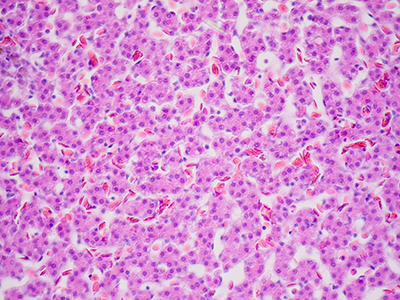
A team led by Children’s National Hospital found that H-IPSE is internalized by just a limited range of cells, including hepatocytes.
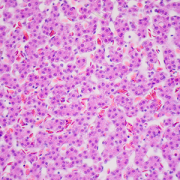
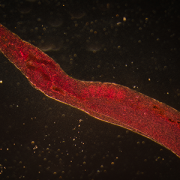
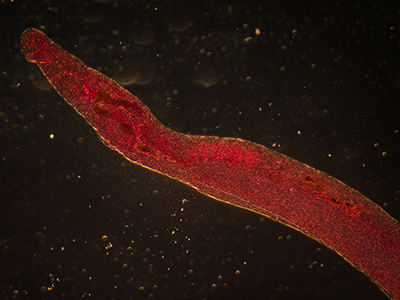
Schistosoma mansoni is a parasite that hides out in snails, breaks free into waterways, and then infects humans, spending much of its life inside blood vessels, laying eggs and jeopardizing public health when those eggs are excreted in urine or feces. As parasitic diseases go, the ailment it causes, Schistosomiasis, is second only to malaria in global impact, according to the Centers for Disease Control and Prevention.
In order to elude the human host’s defenses, S. mansoni uses self-defense tactics that researchers are trying to better understand in order to outmaneuver the parasite. A research team led by Children’s National Hospital is trying to tease out the multiple steps that enable this parasite to reproduce and generate millions of eggs without killing its host.
The parasite’s eggs secrete a number of proteins, with IPSE as one of the most abundant, the team recently presented during the American Society of Tropical Medicine and Hygiene 2019 annual meeting. That protein binds immunoglobulin, which induces basophils and mast cells to release IL-4. After sequestering chemokines, H-IPSE infiltrates the cell nucleus (thus H-IPSE is called an infiltrin), modulating gene expression.
“H-IPSE tips the immune system balance, making it more likely to trigger a Th2 anti-inflammatory response,” says Michael Hsieh, M.D., Ph.D., director of transitional urology at Children’s National and the research project’s senior author. “It downregulates pro-inflammatory pathways, but we wanted to know more about which specific human cells it targets.”
Using Trypan Blue, a stain that selectively colors certain cells bright blue, they solved the mystery, finding that H-IPSE is internalized by just a limited range of cells. What’s more, some cell types, like urothelial cells and hepatocytes (the liver’s chief functioning cells, which activate innate immunity), are more susceptible than neurons, endothelial cells or immature dendritic cells.
In addition to Dr. Hsieh, presentation co-authors include Olivia Lamanna, Evaristus Mbanefo and Kenji Ishida, all of Children’s National; Franco Falcone, of University of Nottingham; and Theodore Jardetzky and Luke Pennington, of Stanford University.