Optimizing pediatric quality & safety in the NICU
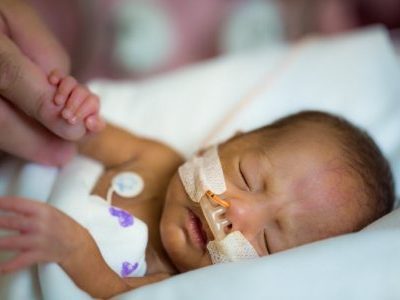
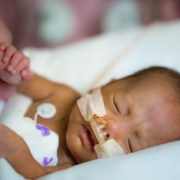
Children’s National doctors are optimizing pediatric quality and safety by working to decrease the rate of hypothermia in the Neonatal Intensive Care Unit.
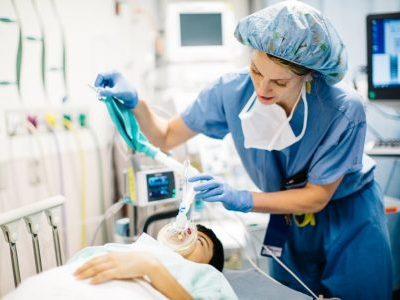
Jessica Cronin, M.D., an anesthesiologist at Children’s National Health System, is working closely with staff and researchers to optimize pediatric quality and safety at the hospital. One of the projects Dr. Cronin is assisting with helps some of the smallest and most vulnerable patients that need surgery. Specifically, she is working to decrease the rate of hypothermia in the Neonatal Intensive Care Unit (NICU).
“It’s a significant problem that children may become cold during the surgery and immediately afterwards,” said Dr. Cronin. “There are a number of complications associated with that occurrence and our doctors and researchers are looking for solutions to combat that issue,” she added.
The hospital staff has instituted several interventions by making data available to the anesthesiologists responsible for temperature management and receiving feedback every month on the types of incidences that are happening. From when a baby is in the NICU, moved to the operating room and when they get transferred back, the doctors at Children’s National have created a checklist of tools to keep babies warm and monitor their temperatures during the perioperative period.
The NICU team has also worked closely with Dr. Rana Hamdy, M.P.H., M.S.C.E., who leads the antimicrobial stewardship team, Sudeepta Basu, M.D., a board certified neonatologist at Children’s National, and the pharmacy team to decrease out antibiotic utilization rates. To achieve its goals, the hospital has implemented the use of real-time check-ins during rounds, new algorithms, de-escalation of antibiotics and the frequent auditing has significantly reduced the unnecessary use of vancomycin.
This project is currently being tested in other parts of the hospital. Furthermore, the Children’s National team recently won an award from the District of Columbia Hospital Association (DCHA) to develop and implement interventions including clinical practice guidelines, educational initiatives, pharmacy-initiated prompts on rounds to de-escalate or discontinue vancomycin review from the antimicrobial stewardship team and provide documentation of culture volumes.
The DCHA serves as the unifying voice working to advance hospitals and health systems in D.C to strengthen systems of care, preserve access and promote better health outcomes for patients and communities. The Children’s National NICU team has been recognized for their outstanding work.
“The work that Dr. Cronin and the rest of the anesthesia team are performing is outstanding,” said Lamia Soghier, M.D., F.A.A.P., C.H.S.E., neonatologist and medical director of the neonatal intensive care unit (NICU) at Children’s National. “Our doctors have cut our rates of hypothermia for postoperative NICU infants by 60% and this project marks one of our major successes!”