Novel technique improved nerve visualization in head and neck surgery
In a pre-clinical model, researchers from Children’s National Hospital found that the Mueller polarimetric imaging, a novel technique that improves image contrast, may help identify nerves from other surrounding tissues during neck and head surgical procedures, avoiding accidental nerve damage.
“This technology holds great promise for the possibility of a truly noninvasive imaging approach and may help improve surgical outcomes by potentially reducing inadvertent, ill effects of nerve injuries in head and neck surgery,” said Bo Ning, Ph.D., R&D engineer at Children’s National and lead author of the study.
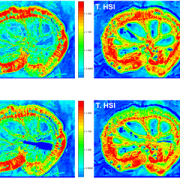
This pre-clinical study presents the first application of a full-field polarimetric imaging technique in vivo during head and neck surgery to highlight the vagus nerve (VN) and a branch that supplies all the intrinsic muscles to the larynx, known as recurrent laryngeal nerve (RLN).
“Unlike conventional nerve identification devices, this technique is noninvasive and less interruptive to intact tissues without disrupting surgical workflows,” said Ning et al. “Since the technique has an easy mechanism and promising performance in our study, this novel method holds great potential for real-time, noninvasive, and convenient nerve visualization.”
While some promising methods use polarimetric imaging for tissue characterizations, the current literature is still limited to ex vivo conditions due to the system complications and prolonged acquisition speeds.
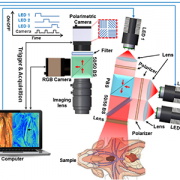
“Recently, the industry released a new polarimetric camera, which is compact and allows fast and high-definition polarimetric imaging through simple snapshots. Enlightened by this technical advance, we have developed a practical polarimetric imaging method,” said Ning, who also develops compact and practical imaging systems for surgical innovation, including 3D, fluorescent, laser speckle and hyperspectral techniques. “It allows fast polarimetric analysis and can acquire birefringence maps over the whole field of view within 100 milliseconds, which provides an appropriate speed for directly surgical use.”
The new approach proofs that the concept is feasible to set up in live subjects during head and neck surgery, which can also be easily adapted for other surgeries. Among the seven subjects, the VNs and RLNs were successfully differentiated from arteries and other surrounding tissues.
Additional co-authors from Children’s National include Itai Katz, Ph.D., M.S., R&D staff engineer III; Anthony D. Sandler, M.D., Senior Vice President and Surgeon-in-Chief; Richard Jaepyeong Cha, Ph.D., research faculty assistant professor.
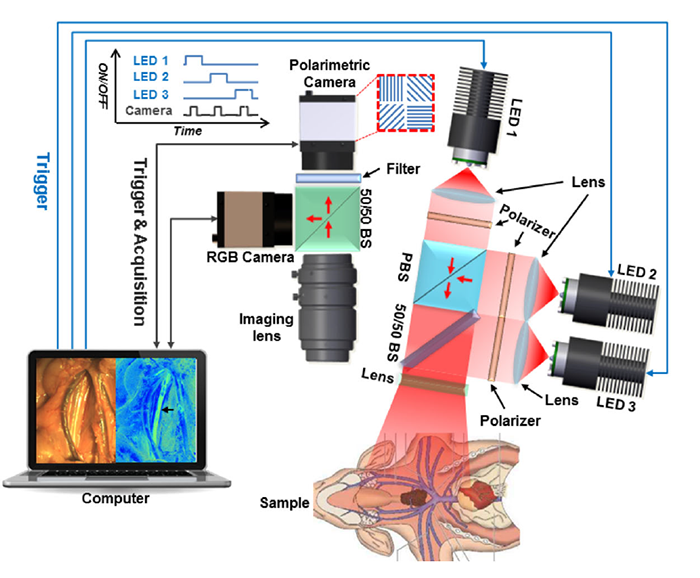
Researchers at Children’s National used a novel technique that improves image contrast, which may help improve surgical outcomes.