Lifesaving ICDs can cause anxiety, stress, PTSD for parents and kids

Research shows that children with implantable cardioverter-defibrillators, and their parents, are at risk for anxiety, post-traumatic stress disorder and other psychological distress.
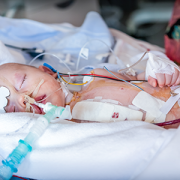
Recent advances in design and efficiency of implantable cardioverter-defibrillators (ICDs) have led to their increased use in younger patients, protecting more children with congenital heart disease from sudden cardiac arrest and sudden cardiac death, says a commentary in the journal Heart Rhythm. However, living longer with these devices and the day-to-day worry that they may have to deliver a lifesaving shock in the blink of an eye, may cause unusually high rates of anxiety, stress and other psychosocial distress for children with ICDs and their families.
Commentary authors Vicki Freedenberg, Ph.D., RN, electrophysiology nurse scientist, and Charles Berul, M.D., chief of cardiology, both from Children’s National Hospital, note that current available research shows both children with these ICDs and their parents are at risk for anxiety, post-traumatic stress disorder (PTSD) and other psychological distress. They highlight a new study published in the same journal that reports data related to prevalence and factors associated with PTSD in children with ICDs and their parents as a good start to better understanding these impacts.
Why it matters
Freedenberg and Berul say that the new study adds important information to an area without a lot of previous research. They also point out that understanding the long-term impacts of life with these devices is critical to ensuring the overall long-term health and wellbeing of both the children with these devices and their families.
What’s been the hold-up in the field?
The development of devices that work for younger children with congenital heart disease, including advances in ICDs and pacemakers, has increased in the last decade. In this time, studies of how these devices work for children have focused predominantly on clinical outcomes and questions related to clinical care.
As survival rates for children have increased, research needs to shift from the study of mortality and clinical outcomes toward understanding the full spectrum of how these devices impact daily life for these children and their families.
Moving the field forward
According to Freedenberg and Berul, the new study importantly includes both patient and parent perspectives, which is a first in this research area. They also offer recommendations for future studies, including the use of comparison groups to allow for generalization of findings. Researchers might also ask research questions to determine whether the device itself or the medical and non-medical factors that often occur simultaneously are more important to predicting mental health and wellbeing.
However, the commentary concludes with the most important takeaway: More research, with specific parameters focused on the impact of clinical interventions, is desperately needed to truly understand all the ways that children and their families are affected throughout life by the clinical care and support they receive.
Read the full commentary, Potential for shock leads to potential for stress, in the journal Heart Rhythm.