Innovative hypoplastic left heart syndrome treatment offers hope for highest risk children
A recently published study in the Journal of Thoracic and Cardiovascular Surgery is a unique report of outcomes for infants treated using a staged surgical approach such as the “hybrid strategy.”
Adopting a staged surgical strategy as the standard of care for medically fragile children with hypoplastic left heart syndrome (HLHS), a critical congenital heart defect, shows promise as an alternative care path for those who may not be ideal candidates for open heart surgery immediately after birth.
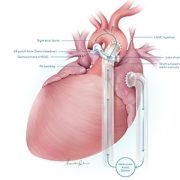
A recently published study in the Journal of Thoracic and Cardiovascular Surgery is a unique report of outcomes for infants treated using a staged surgical approach such as the “hybrid strategy.” This initially less-invasive technique involves the placement of small bands on both lung vessels, with or without the placement of a stent on the ductus arteriosus, as the first stage in surgical palliation.
The study reports results from applying this hybrid approach as a bridge to either a delayed Norwood operation or a comprehensive stage II operation. Over 3.5 years, 30 patients with HLHS were considered very high risk for surgery based on their preoperative risk factors such as low birth weight and/or gestational age, shock, and other medical conditions. During that time, the overall survival rate for this group was 70 percent. In the past, using traditional approaches, the survival chance for infants with HLHS and these high-risk factors was extremely limited.
Why it matters
This new surgical strategy gives the baby extra time to grow and allows doctors to collect detailed analysis of potentially treatable accompanying conditions. Furthermore, high-risk babies recover from birth trauma and have the chance to continue developing crucial organs before undergoing more traditional procedures for HLHS that require open-heart surgery with cardiopulmonary bypass. It also allows surgeons to make an individualized risk assessment for which surgical step should be taken next, replacing the historical “one size fits all” operative pathway for HLHS. The traditional operative pathway for HLHS is a series of three open-heart surgical procedures: the traditional Norwood operation, the bidirectional Glenn and the Fontan.
Advancing the standard of care for HLHS patients beyond the current best practice approach to improve outcomes for more newborns has been slow for several reasons, the authors note. One main reason is that performing a hybrid procedure on these particularly fragile infants requires advanced devices and additional technical expertise. As one example, the authors note that until recently, there was no stent available in the appropriate sizes and with the right material properties to work within such a tiny ductus arteriosus. However, case-by-case expanded access approval by the FDA has brought a new stent designed specifically for this use from Europe to the U.S. for the first time.
What they’re saying
“The Norwood operation revolutionized the care of children with HLHS in the 1980s and gave them a chance for survival,” says Can Yerebakan, M.D., senior author of the study and cardiac surgeon at Children’s National who oversees the hybrid program alongside Joshua Kanter, M.D., director of Interventional Cardiology. “This staged decision-making strategy may give the same kind of hope and offers an alternative pathway of care for high-risk patients who would otherwise have a dismal prognosis and extremely low chance of survival in the newborn period. The success in these cases is, however, based on a multidisciplinary team approach.”
What’s next?
“This strategy not only shows promise for improved short-term survival in high-risk patients, but also boasts the potential to convert some patients to two-chamber circulation instead of one, which our team has done with 100% survival,” says Nicolle Ceneri, M.D., first author of the study and pediatric resident at Children’s National. “As time goes on, we are eager to discover how the use of this approach during such a tenuous period impacts the long-term outcomes for these children and their quality of life.”
Read about the smallest baby born with HLHS to survive to 18 months, who was treated using this hybrid surgical approach at Children’s National Hospital.