Study highlights need for targeted interventions to reduce missed care in pediatric urodynamics
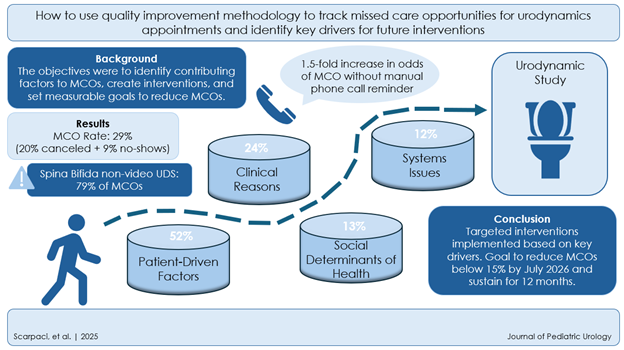
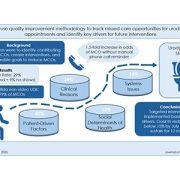
A visual summary of the study’s key findings shows how switching from text reminders to personal calls reduced MCOs in patients with spina bifida, highlighting the importance of tailoring outreach methods based on diagnosis.
A prospective quality improvement study published in the Journal of Pediatrics from the Division of Urology and Spina Bifida Program at Children’s National Hospital reveals a 29% missed care opportunity (MCO) rate in pediatric urodynamics (UDS), with the highest rates seen in patients with spina bifida. Led by a multidisciplinary team, the research tracked 877 scheduled UDS appointments between 2022 and 2024, identifying key patterns that impact care access in this high-risk population.
The study found that patients with spina bifida were especially sensitive to the type of appointment reminder they received. Automated text messages were associated with significantly higher rates of missed care, while human phone calls improved attendance. In response to these findings, the team has implemented targeted reminder strategies and other quality improvement (QI) interventions to reduce MCOs.
What it means
This prospective, condition-specific QI effort aimed to pinpoint not just how often appointments are missed in pediatric urodynamics, but why. Most healthcare systems use standardized reminder systems that don’t account for condition-specific or population-specific differences. This study is one of the first to show how patients with spina bifida – who often require ongoing, multidisciplinary care – respond differently to outreach methods than other patient groups.
By moving beyond a one-size-fits-all approach and identifying the nuanced needs of this population, Children’s National is creating more equitable and effective models of patient engagement.
Why it matters
Missed diagnostic appointments can delay care and increase health risks, particularly in medically complex patients. For children with spina bifida, delays in urodynamic testing can lead to late identification of neurogenic bladder complications, increasing the risk of kidney damage or infection.
“What excites us most is to find that a relatively simple change, switching from automated texts to human phone calls, had a measurable impact on reducing missed care, especially in patients with spina bifida. It showed that small, thoughtful adjustments based on real data can lead to meaningful improvements in access and outcomes for vulnerable patients,” says Kaitlin Scarpaci, DNP, nurse practitioner and advanced practice clinical manager of the Division of Urology at Children’s National Hospital.
How Children’s National is leading
Children’s National is at the forefront of patient-centered quality improvement in pediatric urology. Through close collaboration among advanced practice providers (APPs), physicians and researchers, the institution is actively shaping new care models that reflect the unique needs of medically complex children.
This work builds on the strength of the nationally ranked Urology division and the nationally recognized Spina Bifida Program – both of which are dedicated to ensuring that innovation translates directly into improved care delivery. By investing in prospective data infrastructure and interdisciplinary QI methodology, Children’s National continues to lead the field in actionable, diagnosis-specific solutions.
Additional authors from Children’s National include: Christina Chen, NP, Mary Micker, NP, Hunter Gibbs, PA-C, Perry Harlan, NP, Celicia Little, NP, Nicole Allentuck, Bruce Sprague, Hans Pohl, MD, Christina Ho, MD, Briony Varda, MD
You can read the full study, How to use quality improvement methodology to track missed care opportunities for urodynamics appointments and identify key drivers for future interventions, in the Journal of Pediatric Urology.