“I knew something was wrong because Gabi couldn’t walk in a straight line or ride a bike,” said Gabi’s mom, Petrice Young. “Since the surgery, she’s a different person. Dr. Oetgen literally changed her life.”
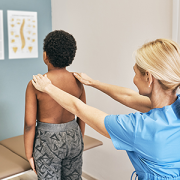
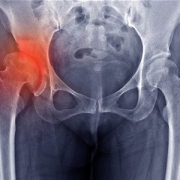
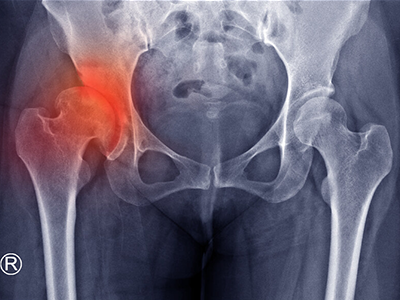
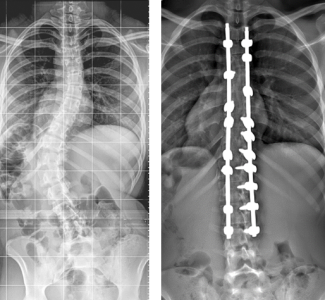
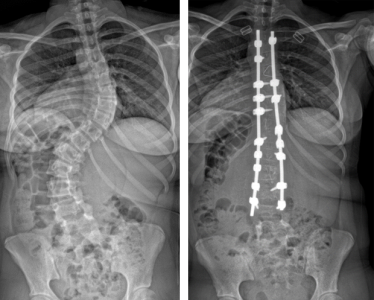
When Gabi, 17, went for her 12-year checkup, her pediatrician noticed a deformity in her spine. He quickly recommended Gabi make an appointment at Children’s National Hospital with Matthew Oetgen, M.D., chief of Orthopaedic Surgery and Sports Medicine. The X-rays indicated Gabi had a very large, 73 degree thoracic and 77 degree lumbar, double-S curvature in her spine and it was likely that as she continued to grow, the curve would get bigger.
Surgery was the best next step. The news came as a surprise to Gabi and her family, especially since she wasn’t experiencing any pain at the time.
“I knew something was wrong because Gabi couldn’t walk in a straight line or ride a bike,” said Gabi’s mom, Petrice Young. “Since the surgery, she’s a different person. Dr. Oetgen literally changed her life.”
Gabi was discharged just four days after her spinal surgery.
As a junior in her high school’s biomedical magnet program, Gabi actively participates as a cheerleader and is currently in her third year as a member of the softball team – something she’d never done before. She maintains a 4.0 GPA and participates in community service regularly.
Her dream career? Becoming an orthopaedic surgeon one day, expressing that her personal experience with the surgery will contribute to fostering a unique and meaningful patient-doctor relationship. She is extremely grateful to Dr. Oetgen for performing the surgery and influencing her career goals.
A program developed to treat the wide range of pediatric spine patients
Since 2015, patients undergoing spinal fusion at Children’s National have been part of the first-of-its-kind pediatric Spinal Fusion Surgical Home care model. This model was developed by a multidisciplinary team with the goal to streamline care for adolescent idiopathic scoliosis (AIS) patients with an emphasis on increasing quality outcomes.
The team’s coordinated approach means they can deliver care more efficiently, resulting in shorter hospital stays and allowing children to come home as soon as it is medically safe. As a leader in this care concept, Children’s National has standardized the infection-control process, pain-management pathway and physical-therapy program for AIS patients who require spinal fusion.
What is AIS?

Gabi actively participates as a cheerleader and is currently in her third year as a member of the softball team – something she’d never done before.
AIS is a condition of the spine, which typically affects children between the ages of 10 and 14 years old, marked by an abnormal side-to-side shaped curve that measures 10 degrees or greater. There are two types of curves associated with idiopathic scoliosis – C-shaped (one curve) and S-shaped (two curves). Along with the curve, the spine also rotates or twists, pulling the ribs along with it. Children with idiopathic scoliosis may experience uneven hips and shoulders and the head may not be centered with the rest of the body.
The period of rapid growth poses the greatest risk for the progression of a child’s spinal curve. Even after reaching skeletal maturity, a child with a curve exceeding 50 degrees may continue to progress at a rate of one to two degrees per year throughout their lifetime.
Treatment of early onset scoliosis
Early onset scoliosis (EOS) is a curve in the spine present before the age of 10. Diagnosing and addressing spinal deformities in children before the age of 10 can significantly impact the long-term outcomes. Close monitoring allows healthcare professionals to intervene promptly if necessary, preventing the progression of the spinal curve.
Minimally invasive techniques are particularly advantageous in pediatric cases, as they often result in shorter recovery times, reduced pain and minimized disruption to a child’s normal activities. This approach aligns with the goal of returning the child to a normal, active life as quickly and seamlessly as possible. Some minimally invasive techniques for EOS include:
- Casting – young children may be placed in what is called Mehta casting. In this advanced casting technique, the child’s chest and abdomen are casted. Every two to four months the cast is replaced as the child grows.
- MAGEC™ (MAGnetic Expansion Control) spinal growing rods – these rods are surgically attached to the spine and doctors use an external remote control outside of the body to lengthen the magnetically controlled rod as the child grows. Traditional growing rods require multiple surgeries.
As part of the Growing Spine Study Group, Children’s National collaborates with other hospitals around the world to enhance care for EOS and related deformities.
The right facility
Children’s National is equipped to treat the most severe and high-risk cases of scoliosis. In rare cases, severe spinal curves can require month-long inpatient spinal halo-gravity traction prior to surgery. This can impede a child’s quality of life just as severely as the condition itself, often making eating, breathing and moving difficult.
Spinal halo-gravity traction can reduce the degree of surgical intervention necessary by accomplishing some gradual straightening of the spine prior to spinal fusion procedures. For severe spinal deformities, this has been shown to improve the safety and effectiveness of the final surgical procedure.
Recognizing the challenges posed by both the condition and its treatment, the surgery team at Children’s National endeavors to coordinate cases, providing patients with mutual support throughout the traction process.
Read more about our advances in Orthopaedic Surgery and Sports Medicine.
 Join Children’s National Hospital for a pre-recorded Continuing Medical Education (CME) presentation on Bracing and Casting in the Pediatric Orthopaedic Surgery Clinic: Improving Patient Care through Understanding and Troubleshooting. This 90-minute presentation will focus on bracing and casting in pediatric spinal deformity, trauma, cerebral palsy and sports medicine. The session offers one (1) CME credit and features Matthew Oetgen, M.D., M.B.A., Jeffrey Peck, M.D., Sean Tabaie, M.D., M.S., M.B.A., and Keyur Desai, M.D.
Join Children’s National Hospital for a pre-recorded Continuing Medical Education (CME) presentation on Bracing and Casting in the Pediatric Orthopaedic Surgery Clinic: Improving Patient Care through Understanding and Troubleshooting. This 90-minute presentation will focus on bracing and casting in pediatric spinal deformity, trauma, cerebral palsy and sports medicine. The session offers one (1) CME credit and features Matthew Oetgen, M.D., M.B.A., Jeffrey Peck, M.D., Sean Tabaie, M.D., M.S., M.B.A., and Keyur Desai, M.D.





 The 2023
The 2023 
 The 2023
The 2023 


 Advanced MRI visualization techniques to follow blood flow in the hearts of cardiac patients. Gene therapy for pediatric patients with Duchenne muscular dystrophy. 3D-printed casts for treating clubfoot. These were among the most popular articles we published on Innovation District in 2023. Read on for our full list.
Advanced MRI visualization techniques to follow blood flow in the hearts of cardiac patients. Gene therapy for pediatric patients with Duchenne muscular dystrophy. 3D-printed casts for treating clubfoot. These were among the most popular articles we published on Innovation District in 2023. Read on for our full list.

 The hospital will advocate for the unique needs of children as part of nationwide network working to accelerate transformative health solutions.
The hospital will advocate for the unique needs of children as part of nationwide network working to accelerate transformative health solutions.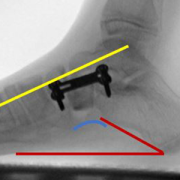
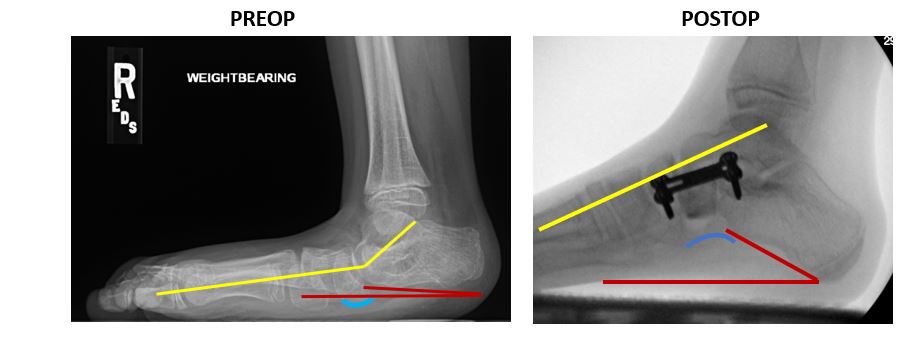 The use of internal brace (IB) augmentation leads to significantly improved long-term foot stability in flatfoot reconstructive surgery for children with cerebral palsy (CP) and pes planovalgus (flat foot) deformities, according to data presented by researchers at the
The use of internal brace (IB) augmentation leads to significantly improved long-term foot stability in flatfoot reconstructive surgery for children with cerebral palsy (CP) and pes planovalgus (flat foot) deformities, according to data presented by researchers at the 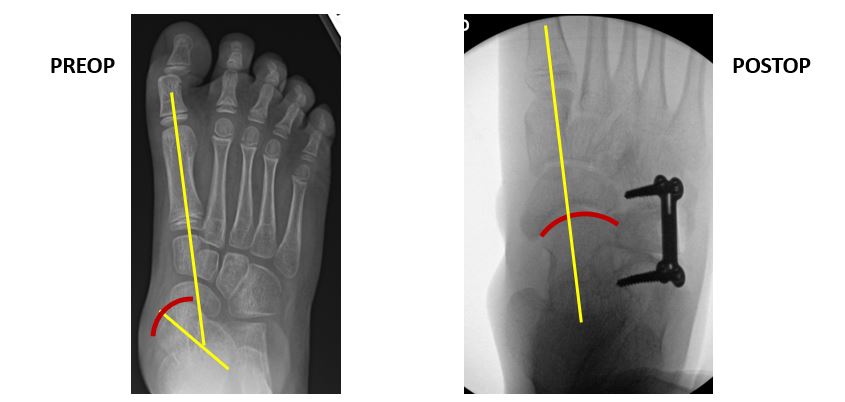

 Children’s National Hospital was awarded nearly $7.5 million in a five-year grant to continue its leadership of an FDA-funded pediatric device consortium. Building upon a decade of previous consortium leadership, the new consortium is Alliance for Pediatric Device Innovation (APDI) and features a new and expanded roster of partners that reflects its added focus on providing pediatric innovators with expert support on evidence generation, including the use of real-world evidence (RWE), for pediatric device development.
Children’s National Hospital was awarded nearly $7.5 million in a five-year grant to continue its leadership of an FDA-funded pediatric device consortium. Building upon a decade of previous consortium leadership, the new consortium is Alliance for Pediatric Device Innovation (APDI) and features a new and expanded roster of partners that reflects its added focus on providing pediatric innovators with expert support on evidence generation, including the use of real-world evidence (RWE), for pediatric device development.


 Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.
Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.