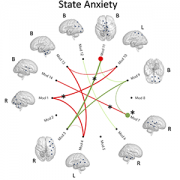
Mothers and their babies often experience stress, depression and anxiety, which impacts the infant’s brain development.
Children’s National Hospital announces a $4.2 million funding award from the Patient-Centered Outcomes Research Institute (PCORI) to support maternal mental health research. The Developing Brain Institute at Children’s National will lead a new program that seeks to advance perinatal mental health and well-being while addressing racial disparities in access to resources that could boost positive health outcomes for women with few opportunities.
Mothers and their babies often experience stress, depression and anxiety, which impacts the infant’s brain development. Maternal psychological distress is more pronounced among low-income mothers — a health disparity that was exacerbated during the COVID-19 pandemic.
“The new fund will support many scientific research portfolios, including our project that will ensure pregnant women in D.C. get the care they need and deserve,” said Catherine Limperopoulos, Ph.D., director of The Developing Brain Institute at Children’s National and co-principal investigator of the project.
“I’m honored to be working alongside Dr. Limperopoulos and our partners. Collectively, our team aims to meet the needs of African American pregnant and postpartum women and their families during this important transition in their lives by providing services to address social determinants of health and prevent and treat maternal distress,” said Huynh-Nhu Le, Ph.D., the co-principal investigator of the project and professor in the Clinical Psychology program, part of the department of Psychological and Brain Sciences at George Washington University.
Cognitive-behavioral intervention, patient navigation and peer support, such tailored strategies developed in the program will provide effective mental health screening and care for 1,000 mothers living in Washington D.C. that is responsive to their cultural, social, environmental, behavioral and medical needs. The participants will access the resources either online or in-person, depending on the type of assistance that fits their lifestyle.
“I am overjoyed that PCORI has provided this essential funding, giving life to our project. The research done here will have a grand effect! Our goals are ambitious: To dissect all aspects of maternal health, beyond just mental health, literally creating a detailed timeline of events a mother can anticipate experiencing from pregnancy, at delivery and postpartum,” said Shanae Bond, one of the women whose firsthand experience giving birth in D.C. informed the study design. “With the maternal health crisis we are currently facing, it’s imperative to gain this type of insight to not only support mothers but to learn how they wish to be supported and how to best improve the care they receive – based on how it impacts, improves (or impairs) their lives,” said Bond.
The multidisciplinary group includes doctors, midwives, psychologists, advisors, community leaders and four prenatal care centers, MedStar Washington Hospital Center, Howard University, The George Washington University and Unity Health Care.
“Our initiative brings together obstetrics, pediatrics, and mental health care in an integrated care model. This collaboration brings early identification and immediate care coordination to its rightful place at the center of care,” said Loral Patchen, Ph.D., CNM, vice chair, Innovation and Community Programs at MedStar Washington Hospital Center. “The prenatal period offers an opportunity for us to support emotional healing, build coping strategies, and offer a safe space for people to prepare for the complex transitions that accompany childbearing. Offering services prior to delivery optimizes opportunity for strong parent-infant attachment and mitigates potential disruptions.”
Kristin L. Atkins, M.D., FACOG, assistant professor in the Obstetrics and Gynecology Department at Howard University College of Medicine, mentioned that Howard University is honored to partner with Children’s National Hospital. “The new program will help discover more about prenatal care interventions related to maternal mental health and how they may impact fetal and pediatric brain development,” said Dr. Atkins. “We are just discovering the impact of long-standing stress on health and well-being, and this starts in utero.”
To Jennifer Keller, M.D., MPH, FACOG, associate professor at The George Washington University School of Medicine & Health Sciences, this project is essential. “The events of the last year have had a profound impact on families in this city,” said Dr. Keller. “This project begins at a time of critical mental health needs for pregnant people in D.C.”
Siobhan Burke, M.D., director of OB/GYN at Unity Health Care, is also thrilled to be part of this partnership. “We all know underlying stressors such as financial difficulties, housing instability and systemic racism can impact health, but it’s important to find out what these things do to the developing fetus and to explore strategies to make lives better,” said Dr. Burke.
In 2020, Children’s National established The Clark Parent & Child Network funded by a $36 million investment from the A. James & Alice B. Clark Foundation. The Clark Network aims to provide families with greater access to mental health care and community resources. New projects like the D.C. mother-infant behavioral wellness program underwritten by PCORI funding will become natural extensions of this essential work.
“This project was selected for PCORI funding not only for its scientific merit and commitment to engaging patients and other stakeholders, but also for its potential to fill an important gap in our health knowledge and give people information to help them weigh the effectiveness of their care options,” said PCORI Executive Director Nakela L. Cook, M.D., M.P.H.. “We look forward to following the study’s progress and working with Children’s National Hospital to share the results.”
This $4.2 million PCORI funding has been approved pending completion of a business and programmatic review by PCORI staff and issuance of a formal award contract.